Immune Support Foundations

For such a complex and increasingly popular topic, my intention is to provide a simple but informative overview of our body’s incredible defense intelligence (the immune response) and factors that influence its performance.
Immune Response Basics
While the core function of the immune system is to perform as a modern day superman, there is the well-known kryptonite, always there to antagonize. The immune system must remain in an incessant position at all times, defending from infection, inflammation, or disease while simultaneously deciding who’s to stay and who’s to go. There are multiple branches of immune regulators such as T regulator cells, natural killer cells, and B cell specific antibodies that act as a 24/7 surveillance system and discerning “Is this self? Or not self? Have we seen this before?” and flagging invaders to be destroyed.
The body maintains both innate immunity; summation of the body’s surface linings, and also adaptive immunity; a further specific targeting system, with immune system cells targeting pathogens (bacteria/virus). The innate immune response is an acute initial process making sure that no known pathogens cross the threshold of the skin and mucous membranes through wounds, abrasions, or contact exposures. However, if a pathogen gains access to the body, this in turn activates the prolonged adaptive response. This adaptive response identifies, targets, terminates, and has the ability of saving to memory the type of bacteria or virus that has been verified, thus making for an enhanced response for subsequent foreign agents.
If this team loses synchronicity or has communication issues, the peaceful and safe neighborhood in your body (known as the microbiome) becomes unregulated making it vulnerable to opportunistic infections, less ready to defend against new pathogens, and the body can go through a bit of an identity crisis presenting as autoimmune diseases, allergies, food sensitivities, and mood disorders.
The smaller known field of psychoneuroimmunology is a fascinating study on these interrelationships that I intend to discuss in a later post!
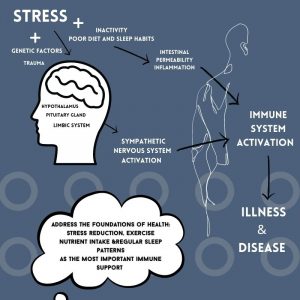
Foundations of Health
Stress Reduction
Currently, research shows that stress is the top proxy causing agent accounting for greater than 60% of all human infectious disease. Yes, it all comes back to stress. Which is why we ALWAYS discuss this our visits and brainstorm stress reduction techniques that resonate with you. Stress is any internal or external stimuli, which causes an innate bodily response. Deciding what is positive stress or negative stress is dependent on the response between the brain (your own perception if something is good for you or not) and your body’s responses over time. Ongoing stressors without adequate maintenance with sleep, rest and relaxation, and mindfulness activities your body can’t keep up work at 100%. Things get faulty and illness is much more likely.
Physical Activity
Exercise/movement/regular physical activity acts as reinforcement for the body’s immune response to stressors and communicable diseases. Being active is one of the main proponents of having a healthy lifestyle. Subsequently, as we age, the body’s immune system loses efficacy, a term known as immunosenescence, so keeping active throughout life is extremely important. Consistent exercise has the ability to improve the function of the immune system cells. Being active regularly, also decreases levels of the inflammatory causing agents related with brain disorders, musculoskeletal disease, and diabetes. Increases of BNDF (brain derived neurotrophic factor) from exercise improves depression, anxiety, memory and learning. Consistency is key! The most important aspect is finding movement that you enJOY. Have fun! Channel that inner child at recess 🙂
Gut Health
Proportionately, about 70% of the body’s immune system cells exist in the intestinal tract, referred to as gut microbiome immunity. This is a balance of the gut microbiome between your “good” probiotic bacteria and the pathogens that reside there. Research studies continue to show probiotics have a beneficial effect on the body’s immune system and have the ability to reduce the severity of respiratory viral infections. When incorporating probiotics into your diet, it’s important to have balance and diversity. The typical misconception about probiotics from the public, are the CFUs (colony forming units), referring to the quantity in one dose. Higher dosage probiotics will often times result in disadvantages for the body to maintain a balanced microbiome. Diversity of the microbiome is most important and comes by way of eating a diverse selection of foods containing probiotics like yogurt and fermented foods, as well as, fiber and prebiotic foods (that act as food for friendly bacteria) such as garlic, onion, asparagus, and chicory. Inflammatory foods such as sugar, fried, and processed foods cause disruption of the immune system and microbiome community. There are many different probiotic products on the market, I would love to find a high quality and effective supplement for you.
Vitamin D
In addition to its role of effectiveness on calcium levels and bone homeostasis, Vitamin D has the ability to act in an immunologic manner by moderating both the innate and adaptive immune responses. We obtain vitamin D through our diet or through synthesis in the skin by way of exposure to UV B light. Some of these various effects on the immune system, include inhibition of B cell and T cell proliferation and the blocking of B cell differentiation and immunoglobulin secretion, resulting in decreased inflammatory cytokine production. Deficiencies in vitamin D are associated with increased autoimmunity and greater susceptibility to infection. Safe sun-light exposure is the premiere source of Vitamin D so getting healthy sun exposure in the summertime can accumulate Vitamin D to help last you through the winter months. However, some people find they are still deficient and supplementation may be necessary (as well as taking note of liver and kidney function that are responsible for activating Vitamin D) Depending on skin type and UV index, too much sun exposure can cause more harm and can give rise to UV-induced immunosuppression and its part in skin carcinogenesis. This is where using sunscreen consciously is important. However, sunlight or UV exposure is still critical to maintain significant levels of Vitamin D and I recommend allowing your body to get uninterrupted rays for 10-20 minutes daily.
Sleep
The relationship between sleep regulating systems (circadian system) within the central nervous system and the cells of the immune system are intertwined. Both the immune and the central nervous system respond to external stimuli, generating memory for the cells; T cells, B cells, Natural Killer cells, and leukocytes (white blood cells). The circadian system and sleep are prominent supervisors of immunological response. Sleep improves the adaptive immune response against an invading antigen and the long-term response of antigenic memory, the staple response of the immune system. Conversely, prolonged sleep deprivation represents a condition of chronic stress which invokes a production of pro-inflammatory cytokines or chronic low-grade inflammation, leading to immunodeficiency. 8 solid hours of sleep is critical to feeling your best and having your immune system primed for action.
Authors: Dr. Nicole Shusterman, ND, Dominique Alexander
References:
1. Anzelone M., ND, Olsen K., ND, Bongiorno P., ND, Lac. (2021, February). Stress, Immunity, and Hair Health. https://www.naturalmedicinejournal.com/journal/2021-02/stress-immunity-and-hair-health
2. The Innate and Adaptive Immune Systems. (2020, July, 3).
https://www.ncbi.nlm.nih.gov/books/NBK279396/
3. Federal University of Fronteira Sul, University of Oeste Paulista (UNOESTE). (2020, July, 29). Physical Exercise as a tool to help the immune system against COVID-19: an integrative review of the current literature. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7387807/
4. Titley, Nick A., M.S. (2014 January). Stress: The Number One Proxy Killer.
https://npionline.org/articles/stress-the-number-one-proxy-killer.htm
DOI: 10.1007/s10238-020-00650-3
5. Sander R. (2012, June, 29). Exercise boosts immune response. https://pubmed.ncbi.nlm.nih.gov/27750511/
DOI: 10.7748/nop.24.6.11.s11
6. Natural Medicine Journal. (2020, May). Enhancing Viral Immunity via the Gut Microbiome
https://www.naturalmedicinejournal.com/journal/2020-05/enhancing-viral-immunity-gut-microbiome
7. Secor E, PhD ND, MPH, MS, LAc. (2016, October). The Immune System: An Integrative Perspective.
https://www.naturalmedicinejournal.com/journal/2016-10/immune-system-integrative-perspective
8. Luciana Besedovsky, Tanja Lange, Jan Born, (2011, November, 10) Sleep and immune function. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3256323/
DOI: 10.1007/s00424-011-1044-0
9. Cynthia Aranow, Feinstein Institute for Medical Research, Manhasset, N.Y. (2011 August). Vitamin D and the Immune System. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3166406/#:~:text=Vitamin%20D%20has%20numerous%20effects,phenotype%5B34%2D35%5D.
DOI: 10.231/JIM.0b013e31821b8755
10. D. H. González Maglio, M. L. Paz, J. Leoni. (2016, December, 13). Sunlight Effects on Immune System: Is There Something Else in addition to UV-Induced Immunosuppression? https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5187459/
DOI: 10.1155/2016/1934518
